Three posts in three days...I guess its safe to say there is alot on my mind.
In followup from yesterdays post, when I mentioned all the good in this world and how I truly believe there is more good than people like to recognize...my friend Jaclyn emailed me today and told me that they were planning the funeral for sweet Gianna and that they were concerned about the expense. The contractor who built the deck on their home, helped make arrangements and they have had the funeral, burial plot and everything else donated to them for free. All of this good will from complete strangers...who still help to bear the grief of their loss. I think this is beautiful. We too have felt so much kindness and goodwill sent our way, and always from the most unexpected sources.
It truly warms my heart in ways you cannot imagine.
Today has been an interesting day. We filled it with garage cleaning, packing up tools for our move. Yes, for anyone who didn't know, we will be moving in the summer, but we still do not know where, as Mickey is still in the interview process. This is a stressful time for him because of course, most colleges will be calling for formal interviews around the same time I will be in Philadelphia, which leaves three small children in need of care, or putting off the interviews which is not ideal either. I just keep hoping that our stent in Philly will be brief, due to having a healthy boy who can come home very quickly.
I truly believe that he is doing so well, and despite the unknown path we take, I feel confident that our miracle is waiting there. This does not mean I do not get discouraged at times. In the past few weeks, several mothers have lost their babies due to hydrops. Another died this morning and I just started getting scared. I am scared...simple as that. I know my journey is not changed by any of these losses, but I truly feel so heartbroken at the loss these mother's are experiencing and I don't want to go through that pain. Its hard to explain and I am not sure anyone who hasn't been through this type of experience can truly relate...I carry within me this beautiful litle boy who has a heart beating strong and long limbs kicking and I have loved him since I first saw those little lines that said POSITIVE....loved him more when I saw his beating heart and loved him more when they told us he was a boy and Oliver danced around the sonography room...my love only continues to grow and I see a future that includes him...
I am scared of losing that future. That life that I desire more than anything, a life that includes my four children in every scene. Mickey reminds me that there is no way to ensure that future includes any of our children, and that I can't do anything more than I am doing to protect it. I know this is true. The future is as unknown for our other kids as it is for Auguste. Everytime I have gotten pregnant I have had that brief wash of dread at the knowledge of loving yet another person with the kind of passion that one can't imagine breathing without them...and yet...that is parenting. I heard said once that parenting is learning to live with your heart walking around outside of your chest.
So ...My four little hearts with thier four little lives and my job as thier mother is to pray that God protects them and keeps them...and trust that He will.
That's a hard task for a control freak like me...and I guess that is why God continues to challenge me with it. I am up for the challenge...and just ask for prayers that I can get better at it, and keep learning to parent gracefully.
(of note, its ironic that my blog ended on that note, because one of the parenting books I have found to be most profound is Grace Based Parenting by Tim Kimmell, if you haven't read it, you should).
kiddos

Saturday, December 29, 2012
Friday, December 28, 2012
Lessons from Loss
 |
| Auggie 32 weeks and 3 days |
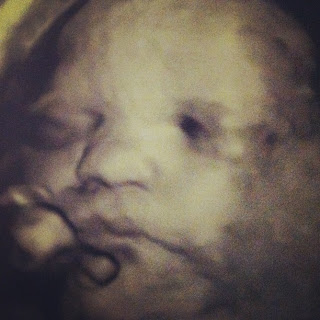 |
| pondering Auguste |
 |
| Bluebird |
 |
| Oliver and Auguste |
 |
| belly shot |
 |
| Family picture taken by my dear friend Julie Blum as she visited from Baltimore |
 |
| Trying to enjoy every bit of my last pregnancy |
On Tuesday, Christmas Day, our Auguste made it to the 32 weeks mark.
I went to the doctor today for an ultrasound and a visit with the maternal fetal docs in Greenville. Things looked really good. His chest was almost completely lear of fluid with only a small amount of fluid at the base of each lung. His abdomen was still distended. Two measurments were taken, one measuring 36 weeks and one measuring 37 weeks and 5 days. A week and a half ago the abdomen measured 35 weeks and 5 days. So, basically it wasn't clear if the abdomen was stable, improved or worse....but Dr. Dillinger was still unimpressed and doesn't seem to be overly concerned regarding the abdomen, stating once again that it is the last to reabsorb. I am of course bothered by it, but I am relieved by the way the chest looks. They estimated the abdomen in the 97th percentile, obviously...and they estimated weight at 6 lbs 9 oz (give or take a lb) and that of course is mostly extra fluid.
Dr. Johnson at CHOP has told me that he has not seen things get worse after 33 weeks, and therefore, I think i will breathe a sigh of relief when things look good next week (wishful thinking)....however, due to the nature of this horrible hydrops, I am not sure I will be at ease until I hear him crying and see him doing well...as I know that all of these babies present differently, and anything can still happen.
However, this is not to say I am not thrilled about the way things looked today.
We took a few more photos. This child has had one to two ultrasounds a week for the past 13 weeks and yet, I can never get a very good photo of him because he HATES the paparazzi. He always holds his hands over his face and is very uncooperative, but here is the latest image of today. The little parts of him we do get photos of are quite beautiful.
Can you believe we have been on this journey for 13 weeks? I have reflected a lot lately about those first few weeks. The idea that termination was recomended, and that had we taken that route we would have never had all these experiences, good or bad...it amazes me. I look at his little face and I thank God that we never considered such a thing. Our lives have been changed so greatly by this little boy and I have to keep pinching myself as the weeks pass and he keeps improving, because I truly never expected things to move this direction. I prayed for it, hoped for it, but truly looked at the reality of the situation and the logical part of me did not think it was possible...and yet, today, on his scan, his lungs looked so big and full and expanded to the chest wall and he keeps kicking at me (which at this point is quite painful) and I dare not complain because I am just so very grateful for every second.
I wanted to post something beautiful written by my friend Jaclyn, after the loss of her sweet Gianna on 12/26/2012. Most of you know that Jaclyn and I met on a hydrops support group page form facebook and became fast friends due to the similarities and the fact that we were both getting treated by the same doctors at CHOP and had due dates in the same window. I am devastated by her recent loss...but her strength in the face of this storm has enocuraged me. I loved how she described what she had learned from carrying a baby with this condition, and it reminds me that every minute is worth it.
What a long journey this has been for my family. Our little girl Gianna Renee Natale was born Dec. 26 at 1:54 pm by c section. I was so scared knowing the out come may not be good. Ii never gave up on my little girl. When the took me in for c section I was given anxiety meds to just keep me calm. Baby was born and my husband was there watching her. The neo natal dr took her right away to try to stabilize her. While i was being sewn up neonatologist told us they were doing everything they could but she wasnt reacting to it. I knew we had to let her go be with the lord. The Lord gave us two hours after she was delivered where she lived and we held her and loved her and kissed her and told her how strong she was and she was our angel. Her heart stopped beating as she was held in her father's arms.
There was no breathing tubes, machines nothing just our girl being taken so peacefully! I am so thankful for those two hours we got with her! The Lord gave us that to remember forever! My heart hurts terribly but I know she has another purpose and the lord needed my angel.
I will never forget this experience as I may not have had much time with my daughter but she taught me so much. She taught me not to be afraid and to face my fears, she taught me to never give up, treasure my family and appreciate every single thing about life and to love until it hurts! She will always be our little girl and im so thankful for this experience!
Thank you everyone for your support. I met a great friend here... Who has been such a support and constant reassurance as she is hurting too she never stopped being a great friend to me! I pray for you all that have traveled the same road as I and i continue to pray for the families that are still fighting there battle! Love to all
— with LisaandMickey Losinski.
There was no breathing tubes, machines nothing just our girl being taken so peacefully! I am so thankful for those two hours we got with her! The Lord gave us that to remember forever! My heart hurts terribly but I know she has another purpose and the lord needed my angel.
I will never forget this experience as I may not have had much time with my daughter but she taught me so much. She taught me not to be afraid and to face my fears, she taught me to never give up, treasure my family and appreciate every single thing about life and to love until it hurts! She will always be our little girl and im so thankful for this experience!
Thank you everyone for your support. I met a great friend here... Who has been such a support and constant reassurance as she is hurting too she never stopped being a great friend to me! I pray for you all that have traveled the same road as I and i continue to pray for the families that are still fighting there battle! Love to all
Thursday, December 27, 2012
Roads Less Traveled
Many many weeks ago, when I was in the first few weeks of this journey, I spoke about calling my Grandfather's voicemail, over and over, and just listening to his sweet voice. The recording of a voice long gone, but one that no one could quite bear to let go of...so the voice still answered the same number I'd dialed a thousand times in my life...the unfailing voices that always answered, always gave support and always prayed. Nearly five years ago my Grandmother no longer answered, and my Pappy stopped answering in August...but his voice remained true in that recording...."God Bless You" he said.
I was so comforted that day, just hearing his voice saying those simple words.
My best friend told me days later that in some of the earliest civilizations, people would call upon those who had gone before them in times of distress, to interecede with God on their behalf.
I haven't shared this before because I have truly been pondering the words of that all this time. The idea of what it means to be made in the image of God. The idea that humanity in its rawest form desires to be closer to God. The idea that no matter what you believe, where you were born, what your worldview is, the most primitive parts of us call out to that higher being when we feel distress.
The instincts of man have always fascinated me. The instinctual way my infant son reached out to hold his infant sister's hand when she cried, the instinctual way we protect our children, the instinctual way we fall in love with one another, and desire companionship and acceptance from one another. The instinctual way we will call out to those who have passed, and to God, to help us and protect us and love us.
Yesterday my friend, who has journeyed with me through this hydrops nightmare, lost her child. She carried her own beautiful baby girl. Protecting her and doing all she could to save her life. Many long weeks added to her child's life due to a mother and father's love and devotion. Two precious hours spent holding her and talking to her before she drifted into Heaven.
We both knew, when we decided to pursue this journey, that the possibility of this ending was great, but it doesn't make going through it any easier.
In those earlier, darker days, my friend became my positive reinforcer, always reminding me how good our babies were doing and how much we had to be grateful for during these extra weeks we offered our babies, and to stay strong and to believe in miracles. It hurts that her journey ended too soon. It makes me reflect on all that we have done and all the hopes we carry with these babies.
I try not to be discouraged, I know that Auguste and I have another road to travel, but it does remind me that I do not know where this road leads me. I can not see the ending and I do not know what lies around the next bend. I just walk in blind faith that I am being led there for a reason, even if I never know what that reason is or why I was chosen to travel it.
And the inner most part of me calls out for guidance, calls out for faith that the path I take won't lead me to more than I can bare, calls out for hope that my miracle is only a few weeks away, and to keep walking towards it, and trust in it. ...
Monday, December 17, 2012
31 weeks
Todays appointment went well. It was nice to have Mickey there with me again. Auguste's little lungs looked good. It has been a while since Mickey has seen them, so for him, it was remarkable improvment. Dr.Dillinger feels they look even better than they did two weeks ago before I left for CHOP. His abdomen is measuring 35 weeks and 5 days, which is not concerning as far as distress at birth, but still perplexing and unclear if it will still resolve or what is actually going on.
Dr. Dillinger did mention that he could not say for sure if any fluid was actually inside the lung tissue, which would cause pulmonary edema, and I had not heard much regarding that yet, so I have some research to do tonight.
I then met with Dr. Twedt, who is wonderful as usual. She once again encouraged me to go to CHOP for delivery and even said that if she were in my situation, that is where she would go as well, which was reassurring.
I also still don't know what we will face after he is born, and I am feeling confident he will live, but I still struggle with not knowing what struggles he will face.
Please pray that his sweet body continues to reabsorb fluid, that his lungs will have proper function when born, and that the ascites will continue to resolve over the coming weeks.
As for the rest of us, I have returned to work and am happy to give the "hydrop obsession" a reprieve. However, I do miss picking kids up from school and our afternoons together. As well as my days with sweet Em. That girl is a mess. She has begun changing out of her pajams every evening after we put her to bed. Tonight she came down in a backward shirt with one hand holding up a pair of Eliot's shorts. Today Oliver developed a fever at school and Mickey went to pick him up. He was sleeping in his teachers lap, which I found so sweet and comforting. The doctor checked both Ollie and Ellie for flu and both were negative, but will still need a few days to rest up. I hope I can get them back soon for their Christmas week events.
This is a busy week and I am just going to do my best to get as many of the things I hoped to accomplish complete prior to the weekend. I have an old friend visiting this weekend and don't want to have too many things on my plate at that time.
Truly, I have so much to say...but really, with all the events of late, feel overwhelmed with the many thoughts and emotions. However, I will say, when people ask where God is during tragedies, or even in cases of sick children, etc...I feel that I see him everywhere. I see him in the people who come to support. I have seen so much love from expected and unlikely places since we found out about hydrops. I see a world currently mourning together and sending so much love to the families in Connecticut. I know we live in a broken world...but God is so many places to be seen...all you have to do is look around and you will see him in the faces of your neighbors, in the faces or your co-workers, patients, friends, children...in acts of charity, in acts of prayer, in acts of mourning...in sweet drawings by children, in music, and in everything beautiful and real in this world.
I truly believe there is much more good in this world than bad. I truly truly believe it and I hope that one day, there will not be trails of separation that keep that love from flowing all the time, and not just as reactions to specific events.
Dr. Dillinger did mention that he could not say for sure if any fluid was actually inside the lung tissue, which would cause pulmonary edema, and I had not heard much regarding that yet, so I have some research to do tonight.
I then met with Dr. Twedt, who is wonderful as usual. She once again encouraged me to go to CHOP for delivery and even said that if she were in my situation, that is where she would go as well, which was reassurring.
I also still don't know what we will face after he is born, and I am feeling confident he will live, but I still struggle with not knowing what struggles he will face.
Please pray that his sweet body continues to reabsorb fluid, that his lungs will have proper function when born, and that the ascites will continue to resolve over the coming weeks.
As for the rest of us, I have returned to work and am happy to give the "hydrop obsession" a reprieve. However, I do miss picking kids up from school and our afternoons together. As well as my days with sweet Em. That girl is a mess. She has begun changing out of her pajams every evening after we put her to bed. Tonight she came down in a backward shirt with one hand holding up a pair of Eliot's shorts. Today Oliver developed a fever at school and Mickey went to pick him up. He was sleeping in his teachers lap, which I found so sweet and comforting. The doctor checked both Ollie and Ellie for flu and both were negative, but will still need a few days to rest up. I hope I can get them back soon for their Christmas week events.
This is a busy week and I am just going to do my best to get as many of the things I hoped to accomplish complete prior to the weekend. I have an old friend visiting this weekend and don't want to have too many things on my plate at that time.
Truly, I have so much to say...but really, with all the events of late, feel overwhelmed with the many thoughts and emotions. However, I will say, when people ask where God is during tragedies, or even in cases of sick children, etc...I feel that I see him everywhere. I see him in the people who come to support. I have seen so much love from expected and unlikely places since we found out about hydrops. I see a world currently mourning together and sending so much love to the families in Connecticut. I know we live in a broken world...but God is so many places to be seen...all you have to do is look around and you will see him in the faces of your neighbors, in the faces or your co-workers, patients, friends, children...in acts of charity, in acts of prayer, in acts of mourning...in sweet drawings by children, in music, and in everything beautiful and real in this world.
I truly believe there is much more good in this world than bad. I truly truly believe it and I hope that one day, there will not be trails of separation that keep that love from flowing all the time, and not just as reactions to specific events.
Wednesday, December 12, 2012
30 Weeks
Yesterday we hit the 30 week mark...unbeliveable and it feels so good. I went to CHOP in the morning and met with Dr. Johnson. He is a doctor I truly do trust. He looked at Auguste and truly felt he was stable from last week and improving. The conversation was extensive, but he said 3 times during the visit that he did not see anything about Auguste that indicated he would die and I should be confident in being able to bring him home one dayd. He is still concerned about the hydrops and the ultimate cause, and encouraged watchful waiting. He has also encouraged delivery at CHOP where he feels that if the fluid does not resolve in utero or right after birth, that they would be ready to find the answers and help him. We enrolled Auguste in a research study involving an umbrella of children who experiences some sort of pulmonary issue beginning in utero. I am a big believer in research and letting Auguste's trials try to help future babies in his current situation.
I took a tour of the NICU and quite honestly, just for a chance to brag on Greenville Hospital, it was not nearly as beautiful as the NICU in Greenville, but it was still nice and large with private spaces and they have ECMO available. The doctors at this point feel it is unlikely Auguste will need ECMO and even feel that due to his effusions being so mild, he may not even experience respiratory distress, but due to the many unknowns we still face, having everything at our fingertips is still reassurring.
Dr. Johnson's only concern seemed to be the million dollar question, what caused this, will it go away on its own, or what will it take to fix it. However, I will once again say that he seemed quite confident that our baby Auguste was going to be one of the 10% of babies that survive hydrops. He believes Auguste will indeed be our miracle. I have to keep telling myself this over and over, pinching myself to make sure it is real.
I flew home last night and finally returned to work today. It felt good to be back with all of my lovely co-workers and to see my sweet patients, all of whom have been praying for me and Auguste in the midst of their own trials. I am truly blessed.
I had a doctors appointment with my OBGYN this afternoon. I let them know all that was going on. Dr. Twedt has been so confident and encouraging and supportive since the first day of this journey, and I feel blessed to have her on Team Auggie. haha.. The entire office for that matter, the nurses and even front office seem happy to see me continueing to walk in the door week after week, and the nurse told me today she hopes I make sure our story gets told. How sweet is that?!
I did discuss frankly with Dr. Twedt the considerations and pros and cons of delivering in Philadelphia, primarily, that they now believe we should go as long as possible, however, I would still need to relocate to Philly at 36 weeks which would mean being away from my family and work for potentially 4 weeks before Auguste is even born. Dr. Twedt still feels that we have come so far, why risk anything now. She said she felt CHOP was the place to deliver because why risk not having ECMO or any other things we may need now. This recomendation did make me feel more confident in delivering at CHOP despite what may happen in the next 6 weeks, but it is still scary.
I do want Mickey to be at the birth, so it is likely we will still consider a 38 week induction. Since our "induction gone sour" with Eliot, I am usually anti-induction for any and all reasons, but I am strongly consdiering it. Emily was born in a matter of hours and if Mickey is in Greenville, he would need a little more notice. My mother is going to try to come nad be with kids during that time, and obviously, since we have no family in town, she will need some notice as well.
As you can see, lots of logistical things that still need to be worked out.
So.....
for now, watchful waiting, trying not to consume too much of my time with all of the statistics and data and fears, continued confidence that God has this under control, and continued prayer that our needs be fulfilled. He is a God of miracles and we are watching those miracles come to fruition.
Christmas is around the corner...the tree is up and stockings are hung and I truly have never felt as blessed as I feel this season.
I want to continue to thank Beth and Stefen and Nico DeWet for continuing to be such wonderful and gracious hosts to me while in Philadelphia. I want to thank all of the people at the Cancer Centers for their support during this. I want to thank my family and of course, all of my friends. The letters and calls and prayers I have continued to receive mean so very much to me. I am truly without words. The kindness we have received has been a miracle in and of itself, and has blessed us so much. Thank you.
Coming home last night to delightful squeals from my kids, and their continued prayers for baby Auggie every night, so innocent, so faithful, and so sincere....my cup runneth over.
I took a tour of the NICU and quite honestly, just for a chance to brag on Greenville Hospital, it was not nearly as beautiful as the NICU in Greenville, but it was still nice and large with private spaces and they have ECMO available. The doctors at this point feel it is unlikely Auguste will need ECMO and even feel that due to his effusions being so mild, he may not even experience respiratory distress, but due to the many unknowns we still face, having everything at our fingertips is still reassurring.
Dr. Johnson's only concern seemed to be the million dollar question, what caused this, will it go away on its own, or what will it take to fix it. However, I will once again say that he seemed quite confident that our baby Auguste was going to be one of the 10% of babies that survive hydrops. He believes Auguste will indeed be our miracle. I have to keep telling myself this over and over, pinching myself to make sure it is real.
I flew home last night and finally returned to work today. It felt good to be back with all of my lovely co-workers and to see my sweet patients, all of whom have been praying for me and Auguste in the midst of their own trials. I am truly blessed.
I had a doctors appointment with my OBGYN this afternoon. I let them know all that was going on. Dr. Twedt has been so confident and encouraging and supportive since the first day of this journey, and I feel blessed to have her on Team Auggie. haha.. The entire office for that matter, the nurses and even front office seem happy to see me continueing to walk in the door week after week, and the nurse told me today she hopes I make sure our story gets told. How sweet is that?!
I did discuss frankly with Dr. Twedt the considerations and pros and cons of delivering in Philadelphia, primarily, that they now believe we should go as long as possible, however, I would still need to relocate to Philly at 36 weeks which would mean being away from my family and work for potentially 4 weeks before Auguste is even born. Dr. Twedt still feels that we have come so far, why risk anything now. She said she felt CHOP was the place to deliver because why risk not having ECMO or any other things we may need now. This recomendation did make me feel more confident in delivering at CHOP despite what may happen in the next 6 weeks, but it is still scary.
I do want Mickey to be at the birth, so it is likely we will still consider a 38 week induction. Since our "induction gone sour" with Eliot, I am usually anti-induction for any and all reasons, but I am strongly consdiering it. Emily was born in a matter of hours and if Mickey is in Greenville, he would need a little more notice. My mother is going to try to come nad be with kids during that time, and obviously, since we have no family in town, she will need some notice as well.
As you can see, lots of logistical things that still need to be worked out.
So.....
for now, watchful waiting, trying not to consume too much of my time with all of the statistics and data and fears, continued confidence that God has this under control, and continued prayer that our needs be fulfilled. He is a God of miracles and we are watching those miracles come to fruition.
Christmas is around the corner...the tree is up and stockings are hung and I truly have never felt as blessed as I feel this season.
I want to continue to thank Beth and Stefen and Nico DeWet for continuing to be such wonderful and gracious hosts to me while in Philadelphia. I want to thank all of the people at the Cancer Centers for their support during this. I want to thank my family and of course, all of my friends. The letters and calls and prayers I have continued to receive mean so very much to me. I am truly without words. The kindness we have received has been a miracle in and of itself, and has blessed us so much. Thank you.
Coming home last night to delightful squeals from my kids, and their continued prayers for baby Auggie every night, so innocent, so faithful, and so sincere....my cup runneth over.
 |
| Buttercup, loves to be dressed up and get nails painted. |
 |
| Beautiful Boy |
 |
| my three buddies |
 |
| Bluebird |
 |
| Boy |
 |
| Daddy and Buttercup |
Sunday, December 9, 2012
Becoming
I read this today and thought it was appropriate for my blog and the way I've been feeling today. I could write a whole blog on this...and thought about it...but it is late and I am tired, so I will just let you read and let it mean what it means to you.
"It doesn't happen all at once," said the Skin Horse. "You become. It takes a long time. That's why it doesn't happen often to people who break easily, or have sharp edges, or who have to be carefully kept. Generally, by the time you are Real, most of your hair has been loved off, and your eyes drop out and you get loose in your joints and very shabby. But these things don't matter at all, because once you are Real you can't be ugly, except to people who don't understand."
— The Velveteen Rabbit
Love you all, keep praying and keep believing, and be REAL!
"It doesn't happen all at once," said the Skin Horse. "You become. It takes a long time. That's why it doesn't happen often to people who break easily, or have sharp edges, or who have to be carefully kept. Generally, by the time you are Real, most of your hair has been loved off, and your eyes drop out and you get loose in your joints and very shabby. But these things don't matter at all, because once you are Real you can't be ugly, except to people who don't understand."
— The Velveteen Rabbit
Love you all, keep praying and keep believing, and be REAL!
Thursday, December 6, 2012
"Resolving Hydrops"
The God of Miracles, Indeed!!!!
29 weeks and 2 days today. 10 weeks and 2 days have passed since the day they told us Auguste had hydrops fetalis and would likely not survive. The past 10 weeks have been full of ups and downs emotionally, a magnitude of testing and procedures, and multiple doctors visits between 2 offices in Greenville, an office in Charlotte, and the Special Delivery Unit at CHOP. Fortunately, the past few weeks have mostly revealed an active baby with stability, but still very sick and the unknown future possibilities have been endless.
The past few weeks have been highly emotional for me. I see friends from my support groups having babies and the challenges they are facing, and suddenly i felt very alone in this struggle. I realized that I will likely be having this baby in Philadelphia and that if he has an extensive NICU stay, I could be alone for a lot of it. Being alone and facing such challenges and emotional trials would be difficult for me to do alone. I cried myself to sleep several nights in a row worrying about all of the unknowns that awaited us. Hydropic babies sometimes survive, but many die shortly after birth, within days, and some only survive after 3 month stays in the NICU. I have been worried and nervous and scared of what awaited me in the future. Mickey refuses to think about worse cases and has been confident that everything will turn out ok, which I am glad he has felt this way, but the reality of the unknown journey ahead of us has been more difficult for me.
I feel fortunate because I truly do have some of the best friends a girl could ask for. I spoke to my friend Jenny and she was able to identify that despite the bvious, it sounded like I was most concerned about doing any of it alone. She and my other close girlfriends have since told me that they have just been waiting for the point at which they were needed...basically setting a command station, and that they planned to be with me through the completion of this journey. This made me feel sucha peace because I realized that the cold nights in the Philadelphia Ronald McDonald House may be a bit warmer with the oldest friends, who are like sisters to me.
Back to Auguste and less about me:
Last week I mentioned that I felt like his lungs looked improved and that some of his lung tissue expanded all the way to the chest wall...on Tuesday, some both me and the doctor felt they seemed even more improved, and abdomen has been stable, measuring 33 weeks and 4 days, which is actually improved since he grew a week but the ascites did not worsen at all (growing into his abdomen, maybe?). On Tuesday I could tell my docs in Greenville were more optimistic about making it to delivery, and they had lots of questions about what to do at that point, which they wanted the docs at CHOPs opinions on.
Today I went to CHOP. I had a list of questions in hand, from my doctors in Greenville, from Mickey, from me. I was seen my Dr. Moldenhauer and she was shocked at the improvement in his lungs. They even looked better today than Tuesday. I asked how we would know that his lungs were developed enough to sustain life, and she said that was impossible to tell until birth, but that she felt very positive by the look of his lungs that they were developing. She actually called the effusions MINIMAL. His ascites was the same, but she said that it is always the last thing to improve. He has no edema (he has never had scalp edema, but even his chest wall edema has resolved). She was so positive and happy about this. She said that he was still a candidate for shunt until 32 weeks, but that she would be very very surprised if our Auguste ever needed shunts and actually expects to see continued improvement. She said that at this point she would no longer even consider his a "hydropic baby", but rather a "resolving hydrops".
I asked for her honest opinion regarding his survival, and expectations with needs in NICU (with the understanding that a lot of unexpecteds can still occur and that we still do not know the underlying cause of the chylothorax). She said that due to the abdominal ascites, she still felt vaginal delivery was possible, but that would still cause some problems due to infants using their abdomen so much to help them breath, however, she felt that it was unlikely he would require ECMO (though still possible) and that he may not even require chest tubes. She predicted a 2-3 week NICU stay. Do you know what that means? It means she predicted a miracle baby boy who we will be bringing home.
I am without words!!! I believe in miracles and I have been praying for a miracle, but the idea that miracle is within my reach is actually palpable now and I am feeling so incredibly blessed!!!
Thank you so much for all of your continued prayers, they are being answered and we are going to get our miracle.
Please continue to pray because we are not out of the woods yet. I now have to be more concerned about mirror syndrome (presenting with similar symptoms, and can be fatal and the onyl way to save me would be to deliver him)...this is a real possibility and could change everything. We are hoping to get me to 37 weeks (last week of January), and then induce...therefore, we have 8 weeks to get through for the best possible outcomes.
I will be seen Tuesday and will then go home and hopefully try to go back to work for a few weeks (maybe a month even) before most likely returning to Philadelphia at 36 weeks and delivering at 37 weeks. There is a possiblility, even in the event of planned delivery, that we may deliver in Greenville. As he improves, he will require less and less...however, in worse case scenario, or need for ECMO, we would have to be transferred to Charleston or Columbia, and therefore, we will probably decide best peace of mind would be to deliver at CHOP with the people who know us and Auguste intimately. I was given a tour of the special delivery unit today. It is a small unit as only the mothers like me, with sick babies deliver there. Each suite has a window into a "mini NICU suite" where all of the interventions, the neonatologist and his practitioner and nurses are at, and the interventions for baby take place right there and the baby is not just whisked away. I think this is what we will decide, but the idea that we have more options now is relieving.
I am just so very happy and feel so much excitment about truly beginning the planning for my baby, my last baby, my baby boy, Auguste.
On a competely separate note, I need prayer for my peace of mind as I plan for the final days of my sweet dog, Noah, my companion for the past 12 1/2 years. He is worsening and my husband told me I should mke arrangements for when I return home. This is upsetting to me, and not something I wanted to do until summer, and certainly not a stress I wanted to add to the stresses I am already going through, but I know the time has come. Pray for peace in my decisions and peace in my heart as I make them.
Love,
Lisa
Friday, November 30, 2012
Hydrops Fetalis
I eventually want to dedicate a tab of my blog to information solely about Hydrops....until I figure that out, I would like to go ahead and post this information, as this is one of the best summaries I have read, and I will add to it as I can.
Auguste has NON IMMUNE Hydrops and cause grossly unknown, alhough his thoracentesis showed 85% white cell count which tells us that the fluid is lymphatic and therefore, we know chylothorax is involved. However, the cause of the chylothorax is still unknown. He was diagnosed at 19 weeks and we know that is happened spontaneously, as his 16 week scan did not reveal any issues.
Because hydrops was found early, his prognosis is considered "poor". That being said, we are almost 29 weeks and he is still stable, active and although he still has a long way to go, he would not be the first child presenting like this to survive and we are cautiously optimistic to what the future holds for him.
Auguste has NON IMMUNE Hydrops and cause grossly unknown, alhough his thoracentesis showed 85% white cell count which tells us that the fluid is lymphatic and therefore, we know chylothorax is involved. However, the cause of the chylothorax is still unknown. He was diagnosed at 19 weeks and we know that is happened spontaneously, as his 16 week scan did not reveal any issues.
Because hydrops was found early, his prognosis is considered "poor". That being said, we are almost 29 weeks and he is still stable, active and although he still has a long way to go, he would not be the first child presenting like this to survive and we are cautiously optimistic to what the future holds for him.
Hydrops Fetalis/Erythroblastosis Fetalis
What is Hydrops Fetalis?
Hydrops fetalis is the name of a condition or symptom. It is not a disease in and of itself, but rather a complication of other conditions. Hydrops fetalis is an abnormal collection of fluid in at least two different fetal compartments. These compartments or spaces can be fluid collection in the abdominal cavity (ascites), around the heart (pericardial effusion), and/or lungs (pleural effusion), or generalized edema or swelling of the skin and throughout the body (anasarca), as well as polyhydramnios (excess amniotic fluid) and placental thickening.
Hydrops can be divided into two major categories or types: immune hydrops - also called erythroblastosis fetalis - and non-immune hydrops.
Immune hydrops is a complicated process that takes place between the baby's blood and the mother's blood. If a mother is Rh negative and her baby is Rh positive, the mother's body can react to the Rh positive factor in her baby's blood as if it were a foreign body, such as a virus. The mother's body will make antibodies to attack this foreign body. These antibodies will destroy the baby's blood cells.
This destuction of the baby's blood cells causes an anemia (low blood count) in the fetus or unborn baby. The fetus tries to make more red blood cells but is unable to make enough to replace the ones being destroyed. Then, the liver, spleen, kidney, adrenal glands, and intestine try to help in making red blood cells to try to keep up with the numbers that are being destroyed. The blood cells produced in these other organs are usually immature and are referred to as erythroblasts. This gives us the synonym for immune hydrops, erythroblastosis fetalis. The organs that are trying to produce red blood cells are also unable to keep up with making enough to replace the ones that are being destroyed. As the organs work harder to keep up they become enlarged and distorted. Eventually, hydrops may develop because of problems with the blood flow to and from these organs. Most cases of Rh incompatibility (Rh negative mom and Rh positive baby) will result in a mild to moderate hemolytic (blood) problem. However, in 20 to 25 percent of cases, a more severe form develops. In these cases, the baby develops general swelling of the body, ascites (fluid in the abdomen), pleural effusions (fluid around the lungs) and tachycardia (increased heart rate), the classic picture of hydrops.
The incidence of immune hydrops has decreased greatly since the introduction of RhoGAM in the 1960's.
Non-immune hydrops makes up about 75 to 90 percent of all cases of hydrops seen today. Non-immune hydrops can be the symptom of a number of congenital conditions.
Just a few of the many known causes of hydrops include:
- Hematologic (blood) problems, such as fetal hemorrhage, disorders in red blood cell production, genetic hemolytic disorders (approximately 10-27 percent of cases)
- Congenital infections such as syphilis, herpes, cytomegalovirus, parvovirus (approximately 8 percent of cases)
- Genetic syndromes (approximately 10 percent of cases)
- Metabolic disorders (falls within the genetic group as these are an inherited disorder)
- Tumors or masses such as diaphragmatic hernia, cystic adenomatoid malformation, sacrococcygeal teratomas or polycystic kidneys (about 10 percent of cases)
- Cardiovascular abnormalities which consists of structural problems with the heart, arrhythmias (heart rate too fast or too slow), or vascular (blood vessel) abnormalities (approximately 40 percent of cases)
Also, more rarely, non-immune hydrops can be caused by problems with the placenta, umbilical cord or the mother's body. In approximately 5 to 8 percent of the cases no known cause can be identified. These are classified as idiopathic meaning the hydrops is the result of an unknown cause.
The incidence of immune hydrops or erythroblastosis fetalis has decreased dramatically since the 1960's due to the introduction of Rh immune globulin or RhoGAM as well as improvements in treatment options. The incidence of nonimmune hydrops is hard to calculate because many cases will result in fetal death and/or miscarriage of the baby, and some will get better on their own, especially when it is the result of an infectious process. The range of incidence is reported at 1 in 1,500 to 4,000 deliveries.
Prenatal Diagnosis of Hydrops Fetalis:
Prenatal diagnosis (before birth) of hydrops is accomplished by ultrasound. An abnormal or increased fluid collection is noted in at least two distinct fetal body cavities or spaces. Examples can include the abdomen, around the heart and/or lungs and in the subcutaneous tissue. In most cases there is also a general increase in the amount of amniotic fluid (polyhydramnios) and the placenta is thicker than normal. If fluid accumulation is seen in only one area, the diagnosis of hydrops cannot be made. Instead. an increased amount of fluid is simply noted in that area. To differentiate immune from non-immune hydrops involves a blood test of the mother that looks for antibodies associated with blood-group incompatibility.
Because cardiac (heart) anomalies or disorders are a common cause of non-immune hydrops, a fetal echocardiogram (ultrasound of the heart) is highly recommended to look for any structural abnormalities or abnormal heart rhythms. Other tests may be done looking for infections, genetic disorders or other congenital issues that have been linked to the development of hydrops. Your obstetrician will refer you to a specialist that handles high-risk pregnancies. These doctors are called perinatologists.
How does Hydrops Fetalis affect my baby?
Hydrops fetalis is a symptom of a problem with the baby. Immune hydrops will rapidly become fatal for the fetus if left untreated. An infant/fetus with hydrops is severely compromised. The earlier this diagnosis is seen the worse the prognosis. Some of these babies may even die before they are born. When the diagnosis of immune hydrops is made, it needs to be treated as an emergency and immediate arrangements are made for treatment. The treatment will be partly dependent on the gestational age at which the diagnosis was made.
There is a 60 to 90% fetal mortality associated with non-immune hydrops. This mortality rate is dependent on the underlying cause. Many of the underlying congenital anomalies (birth defects) have an extremely high mortality rate in and of themselves. Sometimes, no cause is ever discovered but the perinatologist will be aggressively working to try to find out why the baby has developed hydrops. Some causes can be treated, so the doctor will especially be looking to see if there is a treatable cause. Generally, the earlier in gestation that fetal hydrops is seen, the poorer the prognosis.
If the baby survives to delivery, these babies with hydrops have a distinctive appearance at birth. The babies born with hydrops are very swollen with a large round abdomen due to the fluid collection in the abdominal cavity. Often, these infants will have severe respiratory distress or breathing problems due to a variety of causes. Many have lungs that did not develop completely. This is thought to be a result of limited space in the chest due to a swollen liver and a diaphragm that is pushed upward from the fluid that collected in the abdomen. The polyhydramnios (larger than normal volume of amniotic fluid) may interfere with normal fetal breathing movements also. The smaller than normal lung size results in altered blood flow through the lungs, and higher than normal blood pressure in the lungs. This increased pressure in the lungs limits blood flow through them and limits gas exchange with breathing. The lungs need to rid the blood (and ultimately the body) of carbon dioxide and add oxygen into the blood. Many of these babies have fluid collection around the lungs and/or heart, which complicates already compromised breathing and heart function. Another common complication for these infants is severe low blood sugar (hypoglycemia), which is thought to be the result of altered function of cells in the pancreas. The cause of this altered function is not well understood. Hypoglycemia or low blood sugars put these babies at risk for seizures, apnea and potentially brain injury if not treated quickly. If the underlying cause of the hydrops can be linked to anemia, the baby is at an increased risk of developing hyperbilirubinemia. This problem can become severe very quickly and can potentially cause neurologic injury.
How does Hydrops Fetalis affect my pregnancy?
If your obstetrician suspects a problem with your baby, you will likely be referred to a perinatologist. These are doctors who handle high-risk pregnancies. The perinatologist will perform a targeted ultrasound to look at all of the baby's anatomy (the body and it's systems such as heart, lungs, abdomen, head/brain, arms, legs) and assess the location and amounts of fluid accumulation. He or she will be assessing you and your baby to look for the cause of the hydrops, follow the progression of fluid accumulation and monitor the well-being of both of you. Other specialists you may see are a neonatologist, who will care for your baby once he or she is born; a geneticist who will be evaluating the family health history; and any other specialist as necessary to treat the birth defect(s) that have been noted on ultrasound.
Hydrops may be complicated by preeclampsia and/or mirror syndrome (involves pregnancy-induced hypertension or high blood pressure with renal/kidney involvement) in up to 50 percent of the cases of non-immune hydrops. With mirror syndrome, symptoms in the mother mirror the symptoms in the fetus and can be life-threatening for her. Mirror syndrome can happen at any time during the pregnancy and can persist even after the baby is born. The only treatment for mirror syndrome is immediate delivery of the baby and/or when possible, treatment of the fetus to resolve the hydrops. Preterm labor can be a complication of polyhydramnios (as well as preeclampsia).
How is Hydrops Fetalis treated?
Treatment for hydrops is dependent on whether there is a specific diagnosis to treat. Otherwise the treatment is simply supportive or symptom-focused.
Babies with the diagnosis of fetal anemia as the underlying cause of hydrops have good outcomes to fetal therapy. The treatment includes a percutaneous umbilical blood sampling (PUBS) procedure to document the fetal hematocrit and to perform an immediate blood transfusion for the baby. The amount of blood given is calculated using the desired hemotocrit against the actual, the hematocrit of the blood being transfused and the estimated fetal weight. The goal of the initial procedure is a hematocrit to 20 to 25 percent. This procedure is repeated in 48 to 72 hours to bring the hematocrit to 45 to 50 percent. Then, transfusions are done at two- to three-week intervals, with the last one done at 34 to 35 weeks' gestation. These babies should improve before birth.
The treatment protocol for other cases of non-immune hydrops is aimed at the underlying cause. If the underlying cause is known, the benefits and risks of the treatment will be weighed against likelihood of survival. Babies that have not shown improvement before birth should be delivered at a tertiary care center that is able to provide complex resuscitative efforts in the delivery room. Open discussions about palliative care versus aggressive resuscitation can be openly reviewed with you prior to delivery. The plan for care of your baby can be planned with the neonatologist.
For infants without any specific diagnosis, treatment is supportive as we give the baby time to reabsorb all the edema. Often, there are complications like infection and sometimes the baby is unresponsive to the support provided.
The best method for delivery of babies with hydrops is uncertain. To minimize the amount of maternal and fetal trauma, a Caesarean section may be recommended. At delivery, most babies who are being aggressively resuscitated will require endotracheal intubation (the placement of a special tube in the windpipe) for help breathing. Placing the breathing tube can be difficult because of the swelling from the excess fluid. High-frequency ventilation and high airway pressure settings may also be required to provide the baby with enough oxygen. To help the baby breathe, tubes may need to be placed in the chest to help remove fluide from the abdomen and around the lungs.
Special IV lines may be placed. Normally in the umbilical cord there are two arteries and one vein. Umbilical artery catheter is placed in one of the arteries of the umbilical cord. With this special line, fluids can be given, blood pressure can be monitored, and blood can be removed for blood tests. An umbilical venous catheter is placed in the vein of the umbilical cord. With this IV, fluids and medication can be given for a prolonged period of time.
What about surgery?
Some specific anomalies have been treated with fetal surgery (such as congenital cystic adenomatoid malformation and bronchopulmonary sequestration) only if and when the complication of hydrops is seen. You can discuss this option with the perinatologist.
Will I be able to help care for my baby after birth?
Yes. Please ask your baby's nurse about ways to interact with and care for your baby. These babies are typically very ill at birth and will require aggressive treatments. To help in your understanding about what is being done and why ask questions about the treatments and procedures and visit often with your baby.
If you had planned to breastfeed your baby, you can begin to pump and freeze your breast milk while you are still in the hospital. A lactation consultant can assist in answering your questions. Your milk will be frozen and stored in the Neonatal Intensive Care Unit until your baby is ready for it. The NICU has breast pumps and private rooms available to you when you are visiting. You can bring in pictures, small toys, booties and blankets for your baby while he or she is in the NICU.
When can my baby go home?
If the treatment leads to a reversal and the hydrops resolves, the infant may eventually go home. However, for an infant with non-immune hydrops the prognosis is very poor. Your baby must be able to eat enough to maintain and gain weight and breathe effectively by himself or herself before going home. It is important to remember the complication of hydrops has a poor prognosis of survival except for those cases that have a definite cause with established fetal treatment.
What is my baby's long-term prognosis?
Long-term prognosis is guarded. These babies are critically ill even if they do survive to birth. Of the fetuses diagnosed prenatally, only about 20 percent survive to delivery. Of this number, approximately half will survive the neonatal period. Long-term survival for those that make it through the newborn period is based on the underlying cause of the hydrops. The data currently shows an optimistic outlook for those babies who do survive.
Tuesday, November 27, 2012
28 Weeks!!!
Mickey told me this weekend that this was the first time since he met me that I did not look on the brightside. He truly feels everything with Auguste is going to be ok, and he doesn't know why I suddenly look at all angles and see the negatives. I don't believe I am a "bright side of life" kind of girl, and was surprized he even thought that of me. It is possible he felt that ways because I pretend the bad stuff isn't happening and ignore it...but the truth is, I haven't faced many extremely dire situations on a personal level. I think that looking at the brightside of financial struggles, etc...is different than preparing yourself for the possibility of something like losing a child. I feel that I want to experience every little thing this pregnancy offers...good and bad...because I want to know I faced it head on with my head high and let myself learn and be changed by all of this...in the way only true love can do.
This weekend Baby Micah was born and he is having the expected struggle. I was very upset about it because I truly want him to do well. You develop bonds with the mothers and babies who are traveling this journey with you...and I truly feel his survival is a big step in my journey as well. He is imrpoving every day and I feel so happy and excited about another hydrops miracle happening. Read their story at:
http://www.bhamkelleys.blogspot.com/
Today we hit 28 weeks and I feel good! This week is the first week since Auguste was diagnosed that I felt excited about what our future holds. Certainly, I think a lot of this is the nesting that is settling in...but I feel great.
Our visit today went well. The doctor called things stable. His abdomen is measuring large, at about 32 weeks and 4 days, so more than 4 weeks ahead of schedule. However, his lungs looked good. In fact, I personally feel that they looked better than I have seen them. He still has bilateral pleural effusions, but as we observed both lungs, at least a small portion of each of them went all the way to the chest wall. I have never seen his lungs this expanded before.
They are still unconcerned about his abdomen, although this will certainly play into how he is delivered, as currently, his head and abdomen are the same circumference and we would not want to risk him getting stuck in birth canal...which would either mean C-section, or paracentesis (drawing off fluid from abdomen) right before delivery. More questions for CHOP.
They basically do not feel that the ascites will cause any distress at birth for Auguste. However, today, the doctor said "if this was one of your oncology patients, they would probably not be in any distress with pleural effusions this size". Yes, if they don't get better, he will still require chest tubes at birth, etc...but they truly looked better.
The doctor who has seen me on my last two visits, Dr. Dillinger, is also the first doctor who ever met us and told us about hydrops. Last week, I could tell he was surprized to have Auguste still so active and strong 8 weeks from diagnosis. Today, he truly seemed to feel confident we would get to delivery and even seemed relatively positive. I can't wait to get to CHOP and get their opinions and also create a birth plan.
I then went downstairs and got to do the lovely glucose tolerance test. I don't know the results yet, but I assume it will turn out fine. I got to meet with Dr. Twedt, who I adore. I had Emily with me, and basically Emily sat in DR. Twedt's lap and got loved on our entire visit. I told her how I was feeling confident and she was excited and confident with me. Shereiterated to me how HUGE 28 weeks was and how each week from this point is just that much closer to our miracle. I told her how before this pregnancy, I don't think I truly understood what a miracle each of these children truly are. I feel truly blessed and excited once again about the little boy that I truly believe we will be welcoming in home in a month or two.
I even registered, finally. I am still not sure about a shower. A few friends have asked about this and I am not sure I want to do anything like this BEFORE he is born, but perhaps that too will change as he continues to improve. But I felt registering, even if only for some silly little things, was a positive step in the right direction.
After our appointment, I dropped Emily off with Mickey and I stayed downtown for a work related meeting. I had a bit of time to kill and I walked into a store I have been wanting to visit called the Half Moon Outfitters. I walked around, browsing all the great clothes and shoes and flashlights and other fun stuff. I then asked if I could be led to the bathroom, because I am in THAT stage of pregnancy. The guy leading me there laughed and said he was an expectant father and he understood. As I was leaving the store (without any purchases) I said goodbye and thank you and he started talking to me and asked when I was due. I told him Feb. 19, but that it was likely he would be born sooner. He laughed and it turns out, his baby is also due on Feb.19. He asked about the baby and wanted to know what was going on and was sincerely interested in hydrops, etc. He was very sincere and it was great to meet someone who was also expecting a baby at the same time as us. It even made me feel like perhaps, things would continue to improve and maybe we would still get our February birthdate. You just never can tell...but the light at the end of the tunnel seems brighter to me.
I am still hoping to get to CHOP next week, but at this point, we do not have the extra funds for a ticket. I am confident that things will work out though as I should be getting a check by next week. There is also a dear friend of mine who is hosting a fundraiser this weekend...a "Kick-a-thon" that will be kickboxing and resistance training for 90 minutes with all proceeds going towards plane tickets and medical costs. I am excited about it because it may help us, but also it is a great way to get in shape and I want more people to know about CKO and a fun way to get themselves healthy. Its certainly how I plan to get back in shape after baby. Check them out: http://www.facebook.com/CKOGreenville
If I am cleared at CHOP, I do plan to retunr to work. I loved meeting with co-workers tonight. I have always loved my jobs and loved to work, and I truly feel like being back there, with my patients and co-workers will do me a lot of good, even if it is only for a few weeks.
On my way home tonight I was listening to Pandora and I wish I could just put a link to the play list that I got...those closest to me know that the crooning of Eddie Vedder relaxes me and truly makes me feel good...so tonight...I feel, well, even better.
This weekend Baby Micah was born and he is having the expected struggle. I was very upset about it because I truly want him to do well. You develop bonds with the mothers and babies who are traveling this journey with you...and I truly feel his survival is a big step in my journey as well. He is imrpoving every day and I feel so happy and excited about another hydrops miracle happening. Read their story at:
http://www.bhamkelleys.blogspot.com/
Today we hit 28 weeks and I feel good! This week is the first week since Auguste was diagnosed that I felt excited about what our future holds. Certainly, I think a lot of this is the nesting that is settling in...but I feel great.
Our visit today went well. The doctor called things stable. His abdomen is measuring large, at about 32 weeks and 4 days, so more than 4 weeks ahead of schedule. However, his lungs looked good. In fact, I personally feel that they looked better than I have seen them. He still has bilateral pleural effusions, but as we observed both lungs, at least a small portion of each of them went all the way to the chest wall. I have never seen his lungs this expanded before.
They are still unconcerned about his abdomen, although this will certainly play into how he is delivered, as currently, his head and abdomen are the same circumference and we would not want to risk him getting stuck in birth canal...which would either mean C-section, or paracentesis (drawing off fluid from abdomen) right before delivery. More questions for CHOP.
They basically do not feel that the ascites will cause any distress at birth for Auguste. However, today, the doctor said "if this was one of your oncology patients, they would probably not be in any distress with pleural effusions this size". Yes, if they don't get better, he will still require chest tubes at birth, etc...but they truly looked better.
The doctor who has seen me on my last two visits, Dr. Dillinger, is also the first doctor who ever met us and told us about hydrops. Last week, I could tell he was surprized to have Auguste still so active and strong 8 weeks from diagnosis. Today, he truly seemed to feel confident we would get to delivery and even seemed relatively positive. I can't wait to get to CHOP and get their opinions and also create a birth plan.
I then went downstairs and got to do the lovely glucose tolerance test. I don't know the results yet, but I assume it will turn out fine. I got to meet with Dr. Twedt, who I adore. I had Emily with me, and basically Emily sat in DR. Twedt's lap and got loved on our entire visit. I told her how I was feeling confident and she was excited and confident with me. Shereiterated to me how HUGE 28 weeks was and how each week from this point is just that much closer to our miracle. I told her how before this pregnancy, I don't think I truly understood what a miracle each of these children truly are. I feel truly blessed and excited once again about the little boy that I truly believe we will be welcoming in home in a month or two.
I even registered, finally. I am still not sure about a shower. A few friends have asked about this and I am not sure I want to do anything like this BEFORE he is born, but perhaps that too will change as he continues to improve. But I felt registering, even if only for some silly little things, was a positive step in the right direction.
After our appointment, I dropped Emily off with Mickey and I stayed downtown for a work related meeting. I had a bit of time to kill and I walked into a store I have been wanting to visit called the Half Moon Outfitters. I walked around, browsing all the great clothes and shoes and flashlights and other fun stuff. I then asked if I could be led to the bathroom, because I am in THAT stage of pregnancy. The guy leading me there laughed and said he was an expectant father and he understood. As I was leaving the store (without any purchases) I said goodbye and thank you and he started talking to me and asked when I was due. I told him Feb. 19, but that it was likely he would be born sooner. He laughed and it turns out, his baby is also due on Feb.19. He asked about the baby and wanted to know what was going on and was sincerely interested in hydrops, etc. He was very sincere and it was great to meet someone who was also expecting a baby at the same time as us. It even made me feel like perhaps, things would continue to improve and maybe we would still get our February birthdate. You just never can tell...but the light at the end of the tunnel seems brighter to me.
I am still hoping to get to CHOP next week, but at this point, we do not have the extra funds for a ticket. I am confident that things will work out though as I should be getting a check by next week. There is also a dear friend of mine who is hosting a fundraiser this weekend...a "Kick-a-thon" that will be kickboxing and resistance training for 90 minutes with all proceeds going towards plane tickets and medical costs. I am excited about it because it may help us, but also it is a great way to get in shape and I want more people to know about CKO and a fun way to get themselves healthy. Its certainly how I plan to get back in shape after baby. Check them out: http://www.facebook.com/CKOGreenville
If I am cleared at CHOP, I do plan to retunr to work. I loved meeting with co-workers tonight. I have always loved my jobs and loved to work, and I truly feel like being back there, with my patients and co-workers will do me a lot of good, even if it is only for a few weeks.
On my way home tonight I was listening to Pandora and I wish I could just put a link to the play list that I got...those closest to me know that the crooning of Eddie Vedder relaxes me and truly makes me feel good...so tonight...I feel, well, even better.
Sunday, November 25, 2012
To the Babes in My Life
The "nesting" has begun. As I pulled down all the Fall decorations, and started putting up the Christmas ones...I also started inevitable decluttering of spaces. I decided to tackle the closets. I have two daughters and my sister has three, so there is an abundance of girl clothing....and this weekend it was finally time to go through it all and organize it for give away.
This is my last pregnancy. We planned this pregnancy to be our last, and feel strongly that if in the future we still desire more children, we would be blessed to be able to adopt at that time. I want to be able to relish every moment of it. I had planned to fill my free time with pregnancyyoga and pregnancy photos, etc. I never imagined it would be filled with doctors visits, research, and worry.
It was folding all my sweet baby clothing. Bluebird was a preemie and the size of her wee clothing, clothing I recall being so big on her then, now so small they would not fit her doll babies. I imagine that it is possible Auguste will be this small. Our Ollie was never a tiny baby, but I was able to find some newborn stuff that may work when he is here, and at this point, it seems crazy to me that these small clothes may swallow him up.
There is lots of clothing, all packed neatly to pass on to other friends, and I can't believe this chapter of my life is over. No more baby girls. I am excited about the future, but mourn the past a bit.
So...here's to my past babies....and my last baby, who rests and kicks in my stomach.
This is my last pregnancy. We planned this pregnancy to be our last, and feel strongly that if in the future we still desire more children, we would be blessed to be able to adopt at that time. I want to be able to relish every moment of it. I had planned to fill my free time with pregnancyyoga and pregnancy photos, etc. I never imagined it would be filled with doctors visits, research, and worry.
It was folding all my sweet baby clothing. Bluebird was a preemie and the size of her wee clothing, clothing I recall being so big on her then, now so small they would not fit her doll babies. I imagine that it is possible Auguste will be this small. Our Ollie was never a tiny baby, but I was able to find some newborn stuff that may work when he is here, and at this point, it seems crazy to me that these small clothes may swallow him up.
There is lots of clothing, all packed neatly to pass on to other friends, and I can't believe this chapter of my life is over. No more baby girls. I am excited about the future, but mourn the past a bit.
So...here's to my past babies....and my last baby, who rests and kicks in my stomach.
Subscribe to:
Posts (Atom)


































